It was a seemingly ordinary day. I was in the living room talking with my husband Bill, who sat with his arms folded across his chest. Out of nowhere, he looked at me and said, “There’s something wrong.”
That could have meant a million different things, but I knew it was the start of something big. Bill said he felt a lump under his right arm, and although I’m guilty of sometimes dismissing my husband’s health concerns, this time I was worried.
From Bad to Worse
We had just returned from a trip to Portugal. Looking back, it was obvious that Bill was having trouble keeping up as we explored the country, and he complained of being exhausted all the time.
Bill made an appointment to get checked out. I don’t usually go with my husband to appointments, but I felt that he needed me by his side for comfort and support. Being a schoolteacher, the role of the caregiver came naturally to me, and it was a role I gladly jumped into for Bill.
The doctor told him to come back in 2 weeks to see if the lump had grown. When we returned, we learned it had, and rapidly. We went directly to meet with a surgeon, and by the following day, Bill had surgery to remove the lump.
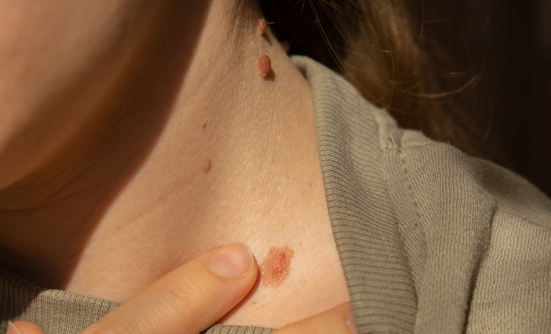
When the biopsy results came back, Bill was given the diagnosis of cutaneous squamous-cell carcinoma (CSCC), a common type of skin cancer. Even before we had the results, we had assumed it was cancer. In our minds, we knew cancer was bad, but we were resolved to do whatever was needed to fix it. However, when the doctor said it was stage IV cancer, which is metastatic cancer, we didn’t know if fixing it was an option anymore.
Listening Is Vital
I’ll never forget when the oncologist told us that the cancer had spread all over Bill’s lungs, his kidneys, his lymph nodes, and under his jaw. The list seemed never-ending. The doctor said that there would be no surgery. There would be no radiation or chemotherapy.
Those first 10 minutes after finding out the severity of Bill’s cancer were the hardest, and I let myself feel and grieve as a wife before switching into the caregiver role.
I had questions and I wanted answers to everything. I knew I had to be listening, really listening, because it was so much information to absorb, and Bill was in a different mental state at the time.
We were told that Bill’s only treatment option was a new immunotherapy drug called Libtayo (cemiplimab), which had just been approved by the FDA for the treatment of patients with metastatic (spreading) CSCC.
First Treatments with Immunotherapy
Bill’s first few infusions of this new immunotherapy were not easy. After the first treatment, he hyperventilated so much that he had to spend the night in the hospital. During the second treatment, I noticed that his face was becoming red and flushed, and I alerted his care team to that, so they decided to stop the infusion.
With the stress of treatment and the diagnosis of metastatic cancer, things were hard for Bill. There was a lot of crying, a lot of “why me?” feelings, and a lot of fear.
Caring for Bill’s Emotional Life

Many people think that a caregiver is mainly in charge of physically caring for a loved one, but so much of what we do involves taking care of the emotional situation. I tried to be a rock for Bill, to talk him through his issues, and calm him down when I could. He often referred to me as his personal psychologist.
A part of my role as caregiver was not leaving him alone for too long. As his wife, I know Bill well, and knew that my absence would be hard on him.
Everybody is different. For some people, it doesn’t matter if their wife leaves for a few hours, but Bill would have felt rejected at that point. It was not always easy to be that rock for him constantly, but I knew that it was what I had to do.
There needs to be a selflessness to caregivers, a willingness to let go of one’s own personal needs most of the time, and to be able to focus on what is best for their loved one. At the same time, you need to take care of your own mental health. This can be a thin line to walk at times.
When I was not feeling able to be supportive to the level that I knew Bill needed, I knew enough to step back and do something helpful to my own psyche. For me, that was reading. Books took me to places outside of the hospital, or away from the bedside, without having to leave Bill’s side. Reading was probably my best source of regrouping.
Finding that outlet was crucial for me.
No Sign of Cancer
By the time Bill had his third treatment, the care team figured out that giving him Benadryl before the treatment, and slowing down the infusion time, made a huge difference. This helped Bill to be able to walk out of the treatment and then drive home, with few or no side effects.
By the fourth infusion, he was feeling more like his old self.
Around that time, Bill had another PET scan, which showed that there was now no evidence of cancer on his kidneys, and the cancer had shrunk dramatically in his lungs. Bill kept receiving infusions with the new treatment, and at his next PET scan a few months later, his oncologist told us that there was no sign of cancer in his body.
There was no protocol for what to do next, because how often do people go from stage IV cancer to cancer-free in a matter of months? We decided that Bill would do 2 more infusions before stopping and seeing what happens. By now he has been cancer-free for more than 1 year, and his next scan is scheduled for January 2021.
Navigating Anxiety
Bill may be cancer-free, but my role as caregiver is not done. He still has to get regular scans, which are hard on him, because he is claustrophobic, and because there is always the fear that the scan will show that the cancer has come back.
Together we’ve also been navigating the anxiety of life during the COVID-19 pandemic, which is common for cancer survivors. Bill’s first cancer-free scan came shortly before the first lockdowns because of COVID-19, which put a damper on our ability to resume life as we once knew it.
Like so many people who are dealing with cancer today, it feels as if our lives are on pause, and sometimes that’s very frustrating, especially because we feared that our lives together would be shortened after Bill’s diagnosis. But like so many other people, we are ready to press “play” when the time comes, and enjoy our time together again.