In 2017, Senator John McCain underwent a physical that revealed a blood clot in his brain. Further assessment confirmed the presence of a glioblastoma (GBM) primary brain tumor. Stories like McCain’s, along with those of other public figures such as Tug McGraw, Scott Hamilton, and Susan Hayward, bring attention to the reality of brain tumors and their impact. Tug McGraw, a celebrated Philadelphia Phillies baseball player and father of country singer Tim McGraw, succumbed to GBM (as did 5 other Phillies players), while Olympic gold medalist Scott Hamilton has faced multiple benign brain tumors since 2005.1
Being diagnosed with a brain tumor requires navigating a cancer journey unlike any other. Brain cancer is a rare and complex disease. In many regions of the United States, accessing expert care is a significant and limiting challenge. Some states lack a single neuro-oncologist—a specialist dedicated to diagnosing and treating brain tumors and other central nervous system (CNS) cancers.2 In addition, the unique anatomical structures of the brain can complicate treatment, with some tumors being inaccessible to surgery and others resistant to treatment medications due to the blood-brain barrier.
The diversity of brain tumors, each requiring tailored interventions, adds another layer of complexity. Rapidly progressing tumors like GBM demand immediate attention and swift action but often come with limited treatment options and no known cure. Beyond the physical challenges, brain tumors can have devastating cognitive and emotional effects. Depending on the tumor’s location, a person’s memory, personality, or very essence can be altered, which is perhaps most heartbreaking for families and loved ones.
This article aims to educate readers about brain tumors, offer an overview of neuro-oncology, and provide patient-focused considerations to help empower individuals to play an active role in their treatment journey. It addresses the unique challenges of the brain tumor experience and offers valuable insights and resources to support families navigating this complex and emotional path. For personalized guidance and support, please consult your healthcare provider and a Brain Tumor Network neuro-oncology navigator for free, one-on-one individualized support.3
About Brain Tumors
Brain tumors are abnormal growths of cells in the brain or central nervous system. They can disrupt essential functions by invading surrounding tissue, compressing critical structures, or interfering with basic brain activity. Understanding brain tumors begins with distinguishing between their different types and recognizing common symptoms.
Types of Brain Tumors
- Primary brain tumors: Primary brain tumors originate within the brain or its immediate surroundings, such as the meninges. Common examples include glioblastoma, astrocytoma, and meningioma. Primary brain tumors can be benign (noncancerous) or malignant (cancerous). Nonmalignant tumors grow slowly and often have distinct borders, whereas malignant tumors are fast growing, invasive, and life-threatening.
- Metastatic (secondary) brain tumors: Metastatic brain tumors result from cancer spreading to the brain from a different source within the body, such as the lungs, breasts, or colon. Metastatic tumors are always malignant and represent the most common type of brain tumor in adults.
For a comprehensive list of brain tumor types, the National Cancer Institute (NCI) provides detailed resources and information online through the NCI-Connect Rare Brain and Spine Tumor Network.4
American Cancer Society’s 2025 Cancer Statistics5
- An estimated 24,820 malignant tumors of the brain or spinal cord are expected to be diagnosed in 2025, with 14,040 cases in men and 10,780 in women
- Brain cancer is the second most common cancer type in children and adolescents at 27% and 22%, respectively
- The 5-year survival rate for brain and CNS cancer is 33%, compared with the average survival rate of 69% across all cancer types
Symptoms
Brain tumors can cause a wide range of symptoms depending on their location, size, and growth rate. Common symptoms include:
- Persistent headaches, often worse in the morning
- Nausea and vomiting without an apparent cause
- Seizures, particularly in individuals without a prior history
- Changes in vision, hearing, or speech
- Weakness or numbness on one side of the body
- Cognitive or personality changes, including memory loss, confusion, or difficulty concentrating
- Balance and coordination difficulties
Recognizing these symptoms, paying attention to your body, and seeking timely medical attention is critical to early diagnosis and intervention. If a brain tumor is suspected, imaging tests are commonly used to confirm diagnosis and guide next steps in treatment planning.
Pediatric Brain Tumors
According to the Pediatric Brain Tumor Foundation, brain tumors are the most common solid tumors in children.6 They present unique challenges due to the developing nervous system and the variety of tumor types—over 120—that can occur in pediatric patients. Common symptoms include headaches, seizures, drowsiness, impaired speech, difficulty swallowing, and vision problems.
Treatment strategies often involve a combination of surgery, chemotherapy, radiation, and targeted therapies. However, the blood-brain barrier, which is a protective layer of cells that acts as a filter, poses a significant obstacle by limiting the delivery of therapeutic agents to the tumor site.
Survivors of pediatric brain tumors face considerable long-term health challenges. By age 50, the average survivor experiences 24 chronic health conditions, the highest among all childhood cancers, compared with 9.2 in the general population. The Pediatric Brain Tumor Foundation offers resources and support for affected families, including educational materials and online support groups. The Brain Tumor Network offers free, knowledgeable navigation support for pediatric patients and families.
Ongoing research aims to develop more effective treatments and improve the quality of life for children diagnosed with brain tumors. Advancements in understanding the genetic and molecular nuances of these tumors are crucial for the development of targeted therapies that can overcome existing challenges.
Diagnosis and Treatment
Diagnosis
The process of diagnosing a brain tumor begins with a thorough medical history and physical examination. If symptoms suggest a brain tumor, additional diagnostic tools may include:
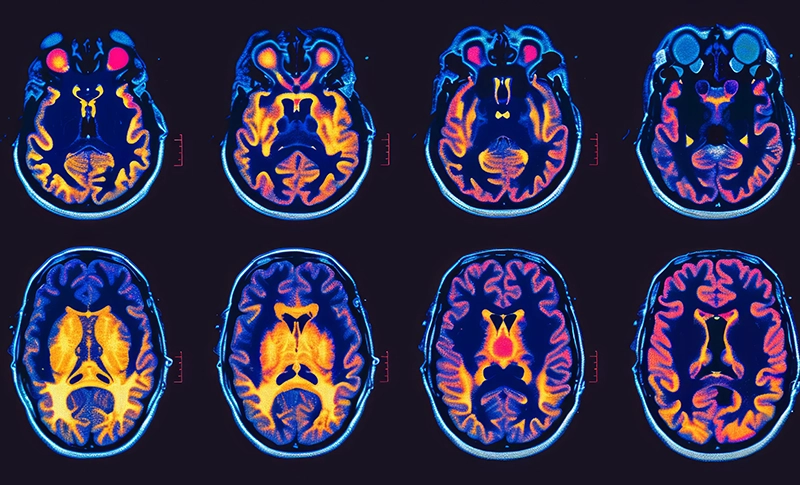
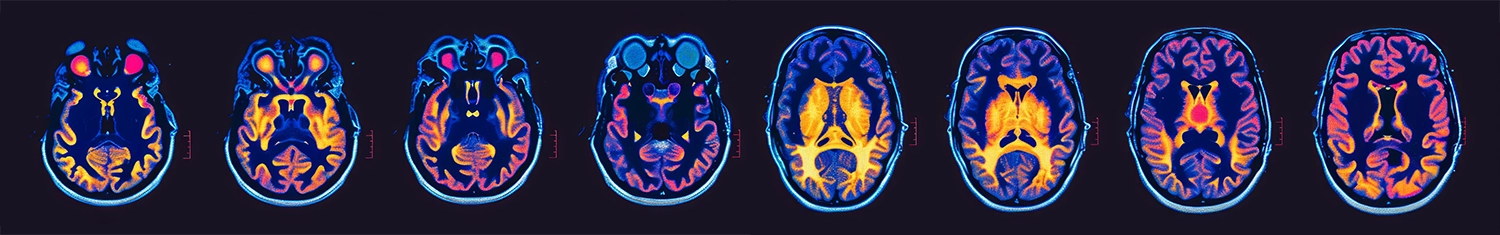
- Imaging tests: Magnetic resonance imaging (MRI) is the most common and detailed imaging technique used to detect brain tumors. Computed tomography scans may also be used in certain cases
- Biopsy: A sample of the tumor tissue is obtained, either through surgery or a minimally invasive procedure, to confirm the diagnosis and determine the tumor type and grade
- Advanced techniques: Functional MRI scans and molecular testing provide detailed information about tumor behavior and genetic mutations
Treatment Options
The first and most important step in deciding on treatment options is to take the time to pause, breathe, and assess your needs before making any hurried decisions. Once a brain tumor is identified, surgery is often emphasized urgently. However, it is essential to remember that the tumor has likely been present for some time—you are now simply aware of it. While immediate interventions are necessary in certain life-threatening situations, not all cases demand the same urgency. Always listen to your healthcare providers, who can guide you in determining whether a prompt response is required.
The first and most important step in deciding on treatment options is to take the time to pause, breathe, and assess your needs before making any hurried decisions.
Seeking a second opinion is another crucial step in understanding all available options, including surgical interventions, medical treatments, and clinical trials. This comprehensive approach ensures that you are making informed decisions about your care.
Consider connecting with an NCI-designated Brain Tumor Center of Excellence for expert brain tumor management. Work with a Brain Tumor Network navigator to identify nearby institutions of excellence, or use the American Brain Tumor Association Brain Tumor Center Search Tool7 to locate potential outlets for care. A multidisciplinary team of specialists, including neurosurgeons, neuro-oncologists, and radiation oncologists, collaborates to create a personalized treatment plan for each patient.
Common treatment approaches include:
- Surgery: Often the first step, surgery aims to remove as much of the tumor as safely as possible. Complete removal may not always be feasible due to the tumor’s growth habit or location near critical brain structures.
- Radiation therapy: High-energy beams, such as protons or photons, are used to destroy tumor cells. This may follow surgery or serve as the primary treatment for inoperable tumors.
- Chemotherapy: Drugs are used to target and kill cancer cells. Chemotherapy can be administered orally, intravenously, or directly into the cerebrospinal fluid.
- Targeted therapy: These treatments focus on specific genetic mutations or molecular targets within the tumor, offering a more personalized approach.
- Clinical trials: Experimental therapies, including immunotherapy, personalized vaccines, and novel drug combinations, are often available through clinical trials, providing access to cutting-edge treatments.
- Supportive care: Symptom management, including seizure control, pain relief, and rehabilitation therapies, plays a vital role in improving quality of life.
The Neuro-Oncology Team: Partners in Care
A brain tumor diagnosis sets patients on a journey that requires the expertise of a comprehensive multidisciplinary team. Each member of the neuro-oncology team brings unique skills to support the patient’s medical, emotional, and logistical needs. Below is an overview of these key roles, along with insights to help patients and families navigate their care.
Neurosurgeon
The neurosurgeon is often the first specialist a patient meets after a brain tumor or anomaly is identified. Their primary role is to evaluate the feasibility and safety of surgical intervention, whether to remove the tumor entirely or obtain a biopsy. However, not all neurosurgeons are experts in brain tumors. In fact, many perform fewer than a handful of brain tumor resections throughout their careers.
Choosing a neurosurgeon with specialized expertise in brain tumor care can significantly impact outcomes. Remember, the surgeon should value the patient as an integral part of the team.
Patients should take the time to discuss their surgeon’s experience with brain tumors during the initial consultation. Ask direct questions about their expertise, such as how many brain tumor surgeries they perform annually and whether they specialize in complex or hard-to-access tumors such as those located at the skull base. Establishing confidence and trust in the neurosurgeon is paramount. Choosing a neurosurgeon with specialized expertise in brain tumor care can significantly impact outcomes. Remember, the surgeon should value the patient as an integral part of the treatment team.
Neuro-Oncologist
Neuro-oncologists are physicians specializing in the diagnosis and management of brain and CNS tumors. They often serve as the primary coordinator of a patient’s treatment plan, overseeing medical therapies such as chemotherapy, targeted treatments, and experimental interventions through clinical trials. Neuro-oncologists also monitor tumor progression through imaging and lab tests.
Patients with brain tumors often benefit from the specialized knowledge of neuro-oncologists, as they are attuned to the unique challenges of these tumors, such as the blood-brain barrier and cognitive side effects, in addition to a high likelihood of familiarity with the latest research and treatment developments in brain cancer research.
Medical Oncologist—What’s the Difference?
Medical oncologists treat a variety of cancers, including metastatic brain tumors, whereas neuro-oncologists focus exclusively on cancers affecting the brain and CNS.
If a neuro-oncologist is not available to you locally, it may be possible to coordinate a second opinion with a neuro-oncology expert, and have them guide your local medical oncologist with recommendations and insights. Talk with your neuro-oncology navigator and insurance provider to learn more about your options. Guidance from a medical oncologist with experience in CNS cancers may be another good option to consider.
Radiation Oncologist
Radiation oncologists design and administer radiation treatments tailored to a patient’s tumor type, location, and size. They employ advanced techniques like stereotactic radiosurgery and proton beam therapy to deliver targeted treatments that minimize damage to surrounding healthy tissue. Radiation oncologists collaborate closely with neurosurgeons and neuro-oncologists to ensure an integrated treatment approach.
Neuropathologist
The neuropathologist plays a critical role behind the scenes. After a tumor is biopsied or removed, the neuropathologist examines the tissue under a microscope to determine its type and grade. Molecular and genetic analyses conducted by neuropathologists provide essential insights into the tumor’s behavior and guide decisions about targeted therapies and clinical trial eligibility.
Neuropsychiatrist
Brain tumors and their treatments can profoundly impact mood, cognition, and behavior. Neuropsychiatrists specialize in addressing these changes, helping patients manage anxiety, depression, and cognitive difficulties. Through psychotherapy and medication, neuropsychiatrists aim to improve mental health and quality of life during and after treatment.
Neuro-Oncology Navigator
A neuro-oncology navigator serves as the patient’s advocate, helping them to overcome treatment obstacles and facilitating access to quality healthcare. From offering education about treatments to assisting with care coordination, the navigator ensures that patients feel supported and informed. Hospitals may employ navigators to assist in appointment coordination and treatment adherence while nonprofit organizations like the Brain Tumor Network provide free, unbiased specialized navigation services to help patients access resources, explore clinical trials, and find expert care.
Social Worker or Case Worker
Social workers are integral to the care team, addressing the practical and emotional challenges of a brain tumor diagnosis. They assist with insurance and financial issues, connect families with community resources, and provide emotional support to both patients and caregivers. Social workers also help families plan for long-term care needs, transitions in care, and much more.
Dietitian
Maintaining proper nutrition is essential for managing treatment side effects and supporting recovery. Dietitians offer personalized guidance to help patients maintain their strength and health, especially during treatments like chemotherapy and radiation, which can affect appetite and digestion.
Physical and Occupational Therapists
These therapists focus on restoring mobility, strength, and independence. Physical therapists help patients regain balance and coordination, while occupational therapists provide strategies for adapting daily activities. Rehabilitation is often a key part of recovery following surgery or other treatments.
Building Your Team
Every patient has the right to a healthcare team they feel confident in. It’s essential to find doctors whose philosophies and approaches align with your goals and needs. To empower yourself in this process, consider using the following resource to prepare for appointments with providers to determine if they are the right fit: National Cancer Institute’s Guiding Questions.8
Click Here for Part II: The Standard of Care for Glioblastoma